|
3/22/2023 0 Comments Cardiac cath guideliner
In a recent study, i-STAT device values were generally 43 seconds lower than Hemochron and 23 seconds lower than the Hepcon devices.For example, Hemochron devices yield higher results than the Hepcon or the i-STAT. typically a low-range card is used for PCI). Target ranges may depend on the device, specific test, and if a high- or low-range calibrating range card is used (e.g.The ACT result is device-specific, even if the activator used is the same (Table 2). 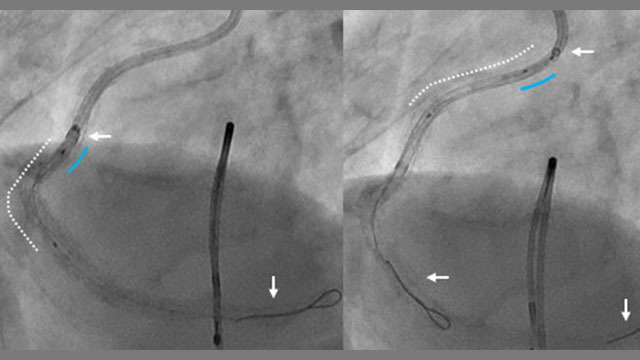
Results can be affected by several factors including platelet count, platelet function, lupus anticoagulants, factor deficiency, testing method, blood volume, warfarin use, technique employed, ambient temperature, and hemodilution.It is predominantly determined by anti-IIa activity and, thus, not reliable to monitor the effect of LMWH, which predominantly inhibits factor Xa.It is typically used to monitor moderate- to high-dose heparin or direct thrombin inhibitor (DTI) doses during invasive procedures, due to the fact that at lower concentrations there is more variability in results.It is generally, a point of care (POC) method, with a normal range of 80-130 seconds.Clotting is initiated in the blood sample by an activator of the intrinsic pathways (such as celite, kaolin, and glass).ACT is a whole blood- clotting time test that initiates clotting and measures the time until clot formation.Overview of the Anticoagulation Monitoring Tests Monitoring and Reversal of Anticoagulation and Antiplatelets. Inactivates thrombin (less affinity) and factor Xa (higher affinity)ĪCT = activated clotting time aPTT = activated partial thromboplastin time IV = intravenous LMWH = low molecular weight heparin POC = point of care subQ = subcutaneous UFH = unfractionated heparin.Īdapted from: Yost GW, Steinhubl SR. Inactivates factors IIa (thrombin) IXa, Xa, XIa, and XIIa Table 1: Anticoagulants for Cardiac Procedures The anticoagulant agents listed (Table 1) have been studied and/or are commonly used peri-procedurally for cardiac cases and meet several of the criteria listed above. 1,2 A point-of-care (POC) test for monitoring, such as during a case, has obvious advantages over a test that requires traditional venipuncture and laboratory measurement. The ideal anticoagulant should have an effect that is of short duration, be easy to monitor, and potentially reversible. 
The following summary is not an exhaustive review and will not discuss the specifics of anticoagulation therapy in depth. In this Tip of the Month, we focus on highlights related to anticoagulation monitoring in the cath lab. In order to optimize the safety of anticoagulation use, operators and cath lab staff need to be aware of the nuances of various tests, testing devices, and therapeutic goals. A key principle when using anticoagulation is to prevent the unintended consequences of bleeding and thrombosis. Beavers, PharmD, BCCP, BCPS-AQ Cardiology, CACP, and Jayant Bagai, MD, FSCAI IntroductionĬath lab procedures, such as percutaneous coronary interventions (PCIs), percutaneous mechanical circulatory support, transcatheter therapies, and ablation, are dependent on the use of anticoagulation therapy to reduce the associated thrombogenic potential.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
